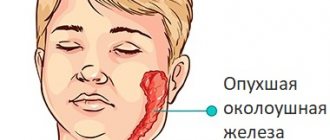
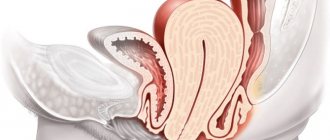
Acute intestinal infection caused by a bacterial environment and characterized by the duration of fever and general intoxication of the body is called typhoid fever. This disease is a severe ailment, as a result of which the main area of damage is the gastrointestinal tract, and when it worsens, the spleen, liver and blood vessels are affected.
Online consultation on the disease “Typhoid.” Ask a question to the experts for free: Infectious disease specialist.
- Causes
- Symptoms
- initial stage
- High stage
- Resolution stage
- Complications
- Diagnostics
- Treatment
- Prevention
The causative agent of this ailment is the microbacterium Salmonella typhi, which is characterized by its resistance to the environment. Entering directly into the human body, this bacterium localizes and releases toxic substances that have a negative effect, causing the corresponding signs and symptoms of the disease.
In the last century, typhoid fever occurred quite often in people, but since the new millennium, cases of malaise have appeared less frequently. But even today, this infectious disease remains not completely eradicated and occasionally doctors diagnose cases of typhoid fever, especially in countries with tense situations (where there are military operations, unsanitary conditions, etc.).
Typhoid fever - what is it?
Typhoid fever is an anthroponotic disease, manifested by the development of severe febrile syndrome, general intoxication symptoms, hepatolienal syndrome, as well as specific roseola rashes and changes in the intestines (ulcerative lesions of lymphoid structures in the small intestine).
In terms of etiology, epidemiological features, developmental pathogenesis and clinical symptoms, the disease is very similar to the paratyphoid group.
Typhoid fever and paratyphoid types A, B and C form a class of typhoid paratyphoid pathologies. For a long time, paratyphoid fever was even described as a mild form of typhoid fever with a blurred clinical picture. For reference. It was found that paratyphoid fever is caused by an independent species of Salmonella, which, unlike typhoid, affects the lymphatic structures of the large intestine and less often leads to the development of severe destructive lesions in the intestine.
According to the ICD10 classification, typhus and paratyphoid fevers are classified as A01. Typhoid fever code according to ICD10 is A01.0.
Typhoid fever is the causative agent
The cause of typhoid fever is typhoid salmonella, which belongs to the genus Salmonella and is part of the family of intestinal enterobacteriaceae.
Typhoid Salmonella are able to survive at low temperatures, but they are highly sensitive to heat. A temperature of 60 degrees kills salmonella in half an hour, and when boiled, typhoid salmonella die in a few seconds.
Attention. The most favorable environment for the proliferation of salmonella is food. In milk, sour cream, cottage cheese, minced meat, etc. The infectious agent can not only persist for a long time, but also actively reproduce.
How can you get typhoid fever?
Typhoid fever is a typical intestinal and anthroponotic infection (that is, only humans can be the source and natural reservoir of the causative agent of typhoid fever).
Both patients with typhoid fever and healthy bacteria carriers pose an epidemiological danger.
The disease is characterized by a pronounced summer-autumn seasonality. Typhoid fever is most often reported in patients between fifteen and forty-five years of age.
Attention. The greatest danger is posed by healthy bacteria carriers or persons carrying typhoid fever in an erased form. Such patients do not know that they are sick and can cause massive outbreaks of typhoid fever, especially if they work with food (food department employees).
The main route of transmission of typhoid fever is fecal-oral. In children's groups, contact and household mechanisms of salmonella transmission can also occur (shared toys).
Patients or carriers excrete Salmonella in feces and urine (in small quantities). Bacteria begin to be actively released into the environment from the seventh day of illness.
Important. Most often, infection with typhoid fever occurs through consumption of water contaminated with salmonella (the pathogen can remain active for a long time in fresh water), milk, sour cream, cottage cheese, ice cream, minced meat (which has not undergone full heat treatment), etc.
Humans have a high level of susceptibility to typhoid Salmonella.
After an infection, stable immunity is formed. In isolated cases, repeated typhoid fever is recorded.
Causes
The causative agent of the disease is the Salmonella typhoid bacillus. When it enters the human body, it releases endotoxin, which is a very dangerous substance.
The pathogen enters the environment through the patient’s urine and feces. Particles of feces on the paws are carried by flies, so the peak of the disease occurs in the summer-autumn period.
Children are most susceptible to the infectious disease, but in adults typhus is more severe and is characterized by an acute onset.
Since this infectious disease is common in third world countries, people who visit epidemic sites, as well as patients with weakened immune systems, are at risk.
Forms of the disease
Based on the nature of the clinical picture, the disease is divided into:
- typically;
- atypical (erased, abortive, outpatient, also includes rare forms - pneumotyphoid, meningotyphoid, nephrotyphoid, colotyphoid, typhoid gastroenteritis).
The pathology can be acute and occur with exacerbations and periods of relapse.
The severity of the infection may be mild, moderate, or severe. Depending on the presence of complications, the disease can be uncomplicated or complicated. Complications of infection may include:
- specific (the occurrence of intestinal perforation with profuse bleeding, shock, etc.);
- nonspecific (the occurrence of pneumonia, parotitis, cholecystitis, thrombophlebitis, orchitis, etc.)
Causes of the disease, its causative agent
The main causes of the disease - typhoid fever - are associated with the entry of Salmonella bacteria into the human body. One of the species, Salmonella typhi, is the causative agent of typhoid fever. This is a very mobile rod with a complex antigenic structure. It exhibits amazing resistance to the external environment in which it is located: bodies of water, dairy products, soil mixtures, the surface of vegetables and fruits.
Destruction of bacteria is possible. To do this, you need to use a 3% chloramine solution or ethyl alcohol. These substances destroy the pathogen; treatment of the disease will not be required in the future.
The main feature of Salmonella bacteria is the complex structure of the typhoid bacillus. The endotoxin it secretes determines the complete clinical picture of the disease.
In some cases, bacteria do not actively manifest themselves, turning into an inactive form. As they fall asleep, they continue to retain their pathogenic properties. And later, due to a decrease in the carrier’s immunity, the diseases become active.
Pathogenesis of the development of typhoid fever
Typhoid fever is an infection with a specific cyclicity and the development of specific pathophysiological changes. Since salmonella enters the body through the mouth, the mucous membranes of the digestive tract serve as the entry point for infection. However, due to the bactericidal effect of gastric juice, if salmonella enters in small quantities, the pathogen can die without leading to the development of the disease.
If salmonella enters the small intestine, it begins to actively multiply and fixate in the lymphoid structures of the small intestine and accumulate in the lymph nodes of the abdominal cavity. The entry of Salmonella into the lymphoid formations of the intestine is accompanied by the development of lymphangitis, mesadenitis, inflammation in the small and sometimes large intestine.
For reference. Damage to the intestinal lymphoid system occurs even before the end of the incubation period of typhoid fever. Subsequently, the pathogen breaks through into the blood, accompanied by the development of severe bacteremia.
Due to the phagocytic activity of leukocyte cells, part of the pathogen dies, releasing endotoxins and causing severe intoxication. At this stage, vivid clinical symptoms of typhoid fever develop: fever, adynamia, drowsiness, lethargy, pallor and cyanosis of the skin, bradycardia, constipation appear, due to paresis of the intestinal muscles, etc.
This period of illness can last from five to seven days. At the same time, part of the pathogen continues to actively multiply in the lymph nodes of the abdominal cavity, maintaining the constant flow of salmonella into the bloodstream and the development of severe inflammation of the lymphoid intestinal formations of the “brain-like swelling” type.
Against the background of ongoing bacteremia, internal organs (tissue of the liver, kidneys, spleen, bone marrow) are affected. This process is characterized by the appearance of specific inflammatory granulomas in them, as well as the development of neurotoxicosis and hepatosplenomegaly (enlargement of the liver and spleen).
Also, the body begins to actively synthesize antibodies to salmonella and the patient develops sensitization, manifested by the appearance of a specific rash. Typhoid fever rashes are foci of hyperergic inflammation in places of greatest accumulation of pathogens in the skin vessels.
Attention! At this stage, the patient is maximally contagious, as he excretes a huge amount of typhoid Salmonella in his feces and urine.
With repeated penetration of bacteria into the intestines, an anaphylactic reaction develops with necrosis of lymphatic tissue.
The severity of bacteremia decreases only in the 3rd week of the disease. In this case, inflammation in the organs persists, and the process of rejection of areas of necrosis in the intestines begins, with the formation of deep ulcers. At this stage of the disease, there is a high risk of developing severe complications: perforation of intestinal ulcers, bleeding and peritonitis.
By the end of the fourth week, the intensity of bacterial circulation in the blood reaches a minimum, body temperature normalizes and the severity of intoxication syndrome decreases.
However, in some cases, typhoid Salmonella can persist in monocytes, leading to distant relapses or exacerbation of the disease. It is also possible that secondary bacterial foci (pyelitis, cholecystitis, etc.) may occur due to the penetration of bacteria into the biliary and urinary systems.
Treatment
Typhoid fever must be treated in a hospital setting. The patient must be isolated from others so that they do not become infected from him. Treatment involves the use of antibiotics and drugs to normalize metabolism, special care and adherence to a strict diet.
Fighting infection
The course of antibiotics lasts throughout the illness until the condition improves.
The most popular drugs in the fight against infection are:
- Levomycetin (4 times a day). Depending on the degree of infection, the dosage may be changed. An antibiotic will eliminate all symptoms, but will not protect against the development of a chronic form.
- In case of secondary symptoms, Ampicillin will be effective.
- If the infection continues to actively develop, then nitrofuran and sulfonamide drugs will come to the rescue.
- In order to exclude relapses, the patient is prescribed non-steroidal anabolics: Methyluracil, Potassium Orotate.
- Antibiotics Ciprofloxacin and Ceftriaxone help improve the condition by lowering body temperature and reducing intoxication.
Taking medications can cause side effects: skin irritation and rashes, stomatitis, vomiting. Individual intolerance may be a reason to discontinue certain types of antibiotics.
Intoxication and dehydration
During the period of illness, the patient's body faces dehydration. At this point, plenty of drinking is required. The patient should drink 2-3 liters of liquid per day.
Sometimes water alone is not enough - drugs from the group of enterosorbents will come to the rescue: Smecta, Polysorb, White and Activated Carbon, Enterodes, etc.
Water, along with medications, helps remove toxins from the blood. Additionally, in a hospital setting, the patient is given a system and a 5% glucose solution is administered intravenously, as well as a solution of Reopoliglucin and Hemodez. They speed up the detoxification process. The norm is 1.5 liters per day.
If glucose-saline solutions do not help, then Prednisolone is prescribed in tablet form for a course of 5 days. When none of the options are suitable and the patient does not get better, they resort to a last resort - a blood transfusion.
Improvement of general condition
The patient requires complete rest and bed rest. He is given a separate room and special hygiene conditions are determined. Bed rest is required for up to 7 days and no more. Otherwise, bedsores will appear on the body. Untimely violation of the regime will lead to muscle tension in the abdominal area and further bleeding and intestinal perforation.
Tincture of ginseng or eleutherococcus will help replenish lost energy and increase the stability of the nervous system.
In order for the body to cope with the elimination of toxins at night, the patient is recommended to drink sleeping pills. This measure also promotes comfortable sleep. Don’t forget about vitamin complexes: A, B, C, E.
Therapeutic diet
During treatment, be careful when choosing food. Nutrition should be gentle on the intestines. It is necessary to exclude perishable and expired foods, spicy and fatty foods. They should not form fermentation processes in the body.
Food should be consumed only light and low-calorie. Better semi-liquid (broth, soup, kefir, liquid cottage cheese) or rubbed through a sieve. Three meals a day in small portions. Doctors also recommend drinking water with your meals.
You need to return to your usual routine gradually. Products not included in the therapeutic diet should be added over 10 days in small portions and not all at once. It is also important to avoid overeating and skipping meals.
Symptoms of typhoid fever
The incubation period for typhoid salmonella ranges from three days to twenty-one days (in most cases from nine to fourteen days). In the period of initial manifestations, the patient experiences general intoxication symptoms: nausea, loss of appetite, weakness, irritability, headaches. In some cases, the disease may begin acutely, with a sharp increase in temperature and severe intoxication.
With a gradual onset, the fever progresses slowly. The maximum increase in temperature (up to forty degrees) is observed on the fifth to seventh day of the disease. In patients with an acute onset, severe intoxication and high fever can be observed already on the second day of the disease.
For reference. Patients with typhoid fever are sharply inhibited, adynamic, and indifferent to what is happening. When you try to talk to them, they give monosyllabic answers after a long pause or do not answer at all. The skin is pale and slightly cyanotic. In some cases, mild facial redness and swelling may occur.
Damage to the cardiovascular system is accompanied by a decrease in blood pressure and a slowdown in heart rate (bradyarrhythmia).
Patients are often bothered by coughing and nasal congestion. When auscultating the lungs, you can hear a lot of scattered dry rales.
Tongue for typhoid fever
Characterized by thickening of the tongue, the appearance of clear teeth marks and a grayish coating on it. At the same time, there is no plaque on the tip and edges of the tongue and their bright red color attracts attention.
There is moderate hyperemia in the pharynx, the tonsils are enlarged.
On palpation of the abdomen, severe bloating and the appearance of a rough, sonorous rumbling in the iliac region are noted. Palpation of the abdomen is sharply painful.
Patients are concerned about severe abdominal pain (manifestation of ileitis and mesadenitis), constipation, nausea, vomiting, and severe weakness. Oliguria (decreased urination volume) gradually develops.
For reference. During the height of the disease, patients are in a state of severe stupor. They do not recognize loved ones and hospital staff, delusions and hallucinations, severe daytime drowsiness and night insomnia, incoherent speech, etc. are noted.
In some cases, small ulcers may appear on the palatine arches (signs of Duguay's angina). By the tenth day of illness, most patients develop reddish-pinkish rashes of a roseolous nature, covering the abdomen, lower chest and, sometimes, limbs.
Important. The rash is strictly monomorphic, that is, it can only be roseola. The number of rashes varies from six to eight (rarely more). The rashes stand out sharply against the background of pale skin. In severe cases of the disease, the rash may be hemorrhagic in nature.
Roseola typhoid rash
The rash lasts from three to five days, after its disappearance there remains a slight pigmentation of the skin. In the future, it is possible to add new elements. In most patients, the skin of the feet and palms acquires a pronounced yellowish coloration (jaundice associated with endogenous carotene hyperchromia of the skin, due to a violation of the conversion of carotene to vitamin A).
Pathogenesis and symptoms during different periods of the disease
The development of infection is quite complex and undergoes several stages.
Table - Pathogenesis of typhoid fever
| Name of period | Characteristic |
| Infections |
|
| Primary local reaction |
|
| The first stages of the disease correspond to the incubation (hidden) phase, which occurs without an obvious clinic | |
| Bacteremia |
|
| Parenchymal spread |
|
| Selection |
|
Sometimes with typhoid fever, after clinical recovery, a person continues to release bacteria into the environment, posing a danger to other people. This variant of the course of the disease is considered a chronic form of infection. This fact is associated with imperfect immune defense.
The clinical course of typhus is divided into four stages.
First phase
Develops immediately after a person is infected with salmonella. The incubation period is considered the most dangerous. It is characterized by the absence of any clinical signs, but the patient releases bacteria into the external environment. The duration of the latent stage of typhoid fever is generally 9–14 days.
The initial period of the disease is characterized by:
- feeling of chills, the temperature curve increases step by step every day, and by the seventh day it reaches 39–41 °C;
- on the part of the nervous system there is marked inhibition and adynamicity, an indifferent attitude towards the environment;
- upon examination, the complexion is pale with slight redness, swelling is observed;
- arterial hypotension, rare pulse;
- unbearable pain in the head, insomnia, decreased appetite up to anorexia;
- Typhoid fever is characterized by hypertrophy of the tongue, the back of which is covered with a grayish-white coating, the tip is bright pink, and on the side parts there are imprints of the patient’s teeth;
- the throat is slightly hyperemic, the tonsils are hypertrophied;
- dyspeptic disorders - bloating, loose stools 2-4 times a day.
When palpating the abdomen, loud rumbling and pain are observed. After seven days, hepatosplenomegaly develops.
Second phase
During the height of infection (5–7 days of illness), clinical symptoms reach their peak.
The prodrome of typhoid fever is characterized by:
- there is a gray-brown coating on the tongue with bright red edges and marks of teeth, the abdomen is swollen evenly due to flatulence and is sharply painful on palpation;
- intestinal function is impaired - repeated loose stools are observed in the form of pea soup with a sour odor;
- severe endotoxicosis - severe fever 39–40 °C, unbearable headache, adynamia, apathy, impaired consciousness with the development of stupor or coma, delusional hallucinations;
- by the tenth day, half of the people develop a scanty roseola rash (exanthema) in the area of the anterior wall of the abdomen or on the lower part of the chest;
- parenchymal jaundice may develop, the liver and spleen are enlarged and clearly palpable;
- Bradycardia, bifurcated pulse, low blood pressure, muffled heart sounds are noted, and systolic murmur is heard.
Symptoms of a focal form of pneumonia often occur, renal function is impaired and oliguria and anuria develop.
Periods of resolution and recovery
The temperature response gradually decreases, sleep normalizes, appetite improves, dyspeptic symptoms disappear, and diuresis increases. The resolution period for typhoid fever is about a week.
Then the person’s gradual recovery begins. The altered functions return to normal and the body is rapidly freed from infectious agents. After suffering from typhoid fever, asthenia in the body persists for a short time, which eventually disappears without a trace.
The occurrence of exacerbations and relapses of infection
During the period of decreasing intensity of clinical symptoms (until the fever disappears), exacerbations may develop. In this case, the patient’s symptoms of fever begin to increase again, roseola rashes, lethargy, etc. appear. In most cases, exacerbation of typhoid fever occurs sporadically.
Multiple exacerbations are extremely rare and are observed with improperly prescribed treatment or in patients with immunodeficiency conditions.
Relapse of the disease is diagnosed when symptoms of the disease appear against the background of normal temperature and the complete disappearance of manifestations of intoxication. Relapses of the disease may be associated with the use of chloramphenicol, which acts on the pathogen bacteriostatically (suppresses growth and reproduction), and not bactericidal (kills the pathogen).
For reference. Relapses can last from a day to ten to fourteen days and are much milder than the disease itself.
Pathogen and its description
The causative agent of typhoid fever is the gram-negative bacillus Salmonella typhi, which belongs to the genus Salmonella, family Enterobacteriaceae. These microorganisms are usually unpretentious and affect not only humans, but also some animals.
It is worth noting that these bacteria, once released into the external environment, can retain the ability to live for quite a long time. For example, salmonella live in soil from 1 to 5 months. On food they remain pathogenic for several weeks. Heating has a detrimental effect on the microorganism, causing its death (this is why pasteurization and proper heat treatment are so important). Pathogenic microorganisms can also be destroyed using disinfectants in normal concentrations.
Diagnosis of typhoid fever
Blood for typhoid fever to isolate blood cultures of typhoid salmonella can be tested from the fifth to seventh day of the disease. Also, analysis for typhoid fever can be carried out using the Widal reaction, detection of specific typhoid antibodies using the RNGA method, as well as detection of immunoglobulins M using ELISA.
Examination of feces and blood using PCR can detect deoxyribonucleic acid of typhoid Salmonella.
From the 2nd week of the disease, RNGA and the Widal reaction are performed, as well as the isolation of typhoid Salmonella cultures from bile, urine and feces.
Complications
Anemia is a possible complication caused by typhoid fever
Typhoid fever, in addition to all that has been said, can cause more unpredictable complications, which are characterized by the occurrence of such serious diseases:
- anemia;
- intestinal hemorrhage;
- perforation of the intestinal wall;
- peritonitis;
- myocarditis;
- thrombophlebitis.
If a patient with typhoid fever spends all the time in bed, then this is fraught with the appearance of bedsores. In order to prevent complications of typhoid fever, it is necessary to promptly seek help from a doctor who will make a diagnosis and prescribe appropriate methods for getting rid of the disease.
Treatment of typhoid fever
All therapy for typhoid fever is carried out exclusively in infectious diseases hospitals. Treatment is comprehensive and includes etiotropic (typhoid vaccine) and antibacterial therapy.
For the treatment of typhoid fever, preference is given to ceftriaxone, cefixime, ciprofloxacin, ofloxacin, and pefloxacin. Antibacterial therapy is carried out for a long time (up to ten days after stabilization of the patient’s temperature).
For mild forms of the disease, azithromycin can be used.
Detoxification therapy with solutions of Ringer, reamberin, rheopolyglucin, etc. is mandatory.
Symptomatic therapy is aimed at maintaining blood pressure, relieving hypothermia, and preventing and treating complications.
For reference. The duration of treatment for typhoid fever is at least twenty-five days (for mild forms of infection). All this time, patients must remain in the hospital. In severe cases of the disease, the duration of treatment can be more than forty-five days.
Forecast
The prognosis depends on whether the infected person is treated promptly with antibiotics. When treated with antibiotics, the prognosis is good, with less than 1% of people dying due to infection. Without antibiotic treatment, the outlook may be poor and 10-20% of people will die due to complications.
Vaccination is also available to provide protection against typhoid fever. Because this is rare in Russia, vaccination against typhoid fever is not usually provided as part of the childhood immunization program.
It is recommended to get vaccinated if traveling to parts of the world where typhoid fever is common.
Main symptoms
Typhus - what kind of disease is it? Let's look into this further. Now I would like to consider the main symptoms that will appear in a person if he is infected. It is definitely worth noting that signs of the disease will not be noticeable immediately after infection. So, they will appear on average at 7-14 days of disease development. In this case, a person may feel:
- Constant headache.
- Increased body temperature.
- Stomach ache.
- Stool disorders. Most often, there is initial constipation, followed by loose stools.
- Patients often develop a dry cough.
- Pink spots may appear, which are mainly concentrated on the back, stomach, and also on the chest.
Ways of transmission of the disease
Typhoid fever is an anthroponotic disease. A person can be a carrier of dangerous bacteria for a long time without having symptoms. There are three main routes of transmission of typhoid fever.
Methods of entry:
- Through contaminated water.
- When consuming contaminated products.
- From person to person.
In children, typhoid fever often occurs as a result of communicating with a sick child or when sharing toys and household items. Infection also occurs through contact with the same dishes, bedding, and household items. Typhoid fever is often transmitted by airborne droplets.
Water poisoning occurs when swimming in natural bodies of water. Often various waste and sewage waters are drained into them.
Raw milk can provoke the disease. In such a product, bacteria multiply quickly, and once they enter the body they disrupt the functioning of internal organs. It is recommended to remember that milk must undergo heat treatment, only after which it can be used for preparing other dishes.
Typhoid fever can develop after eating poor quality food. Flies can carry dangerous bacteria on their legs. It is required to follow the rules for preparing and storing food to avoid intoxication.
Reasons for development
Typhoid fever in children and adults develops as a result of penetration of the pathogenic microorganism Salmonella typhi into the body. The routes of transmission of infection have already been well studied. This microbe is capable of causing disease only in humans. The reservoir of infection is infected people who suffer from this pathological condition or are carriers.
Characteristics of the pathogen
Salmonella typhi is a gram-positive aerobe. This organism is a mobile rod with 10 to 12 flagella. This microorganism is not capable of forming capsules or spores. At the same time, to acquire resistance to the body’s environment, the pathogen can flow into L-cell forms. This is a temporary cell-free state. In this form, this stick becomes resistant to many drugs.
Salmonella typhi has O- and H-antigens in its structure. At the same time, a special virulence antigen was identified in Salmonella of this variety, that is, there is a high probability of mutational transformation of the organism.
Salmonella typhi is characterized by low resistance to chlorine-containing solutions and alcohol. Moreover, these bacteria are capable of surviving and multiplying for a long time in the natural environment and some food products. These representatives of the Salmonella genus tolerate low temperatures well.
Boiling leads to the rapid death of these microorganisms. When these microorganisms enter the human body, they infect the intestines and cells of the lymphatic system, beginning to multiply rapidly. The incubation period for the development of the abdominal type is from 10 to 14 days.
How is it transmitted?
There are several routes of transmission of the causative agent of this infectious disease. Most often, bacteria are transmitted through household contact, that is, through direct contact with an infected person. In addition, pathology can occur when sharing household items and hygiene items that have been exposed to physiological fluids and feces contaminated with pathogenic microflora. In children's groups, the spread of salmonella often occurs through contaminated toys.
Focal typhus epidemics often occur when people use contaminated water from sources that do not undergo special chemical treatment. Such sources include not only rivers and lakes, but also wells and wells. In this case, people who consumed water from contaminated sources, as well as their relatives who were in close contact with the sick, are often found to be affected.
Among other things, transmission of salmonella can occur through contaminated food. Food that has not undergone heat treatment is especially dangerous. The spread of infection often occurs from people who are carriers of the infection and work in the food service industry. There are cases of intrauterine transmission of infection from women who were carriers to children. This type of transmission of salmonella is extremely rare.
Features of treatment
If there is the slightest suspicion of typhoid fever, urgent hospitalization of the patient in the infectious diseases department is required. It is very important to properly establish the patient’s daily routine. To prevent the development of complications, bed rest is prescribed until the 7th day of temperature normalization. The patient is allowed to walk only after 10-12 days of normal temperature.
It is important to follow a strict diet. In this case, the food must be liquid, pureed, easily digestible and contain all the required vitamins. Usually the patient is prescribed fermented milk products, broths, liquid cereals, chopped meat, and juices.
Typhoid fever cannot be treated without taking antibiotics. Typhoid bacillus is very sensitive to ampicillin, as well as its derivatives, in particular, Biseptol or Levomycetin. In addition, there is a special vaccine. The severity of the disease is due to endotoxin, which is why infusion therapy is performed. According to indications, cardiovascular medications, vitamins and sleeping pills may be prescribed.
Traditional medicine gives good results, but they must be used in combination with medications. You should also consult your doctor first.
Notes
- Song J, Willinger T, Rongvaux A, Eynon EE, Stevens S, Manz MG, Flavell RA, Galán JE.
A mouse model for the human pathogen Salmonella typhi. — Cell Host Microbe. 2010 Oct 21;8(4):369-76. - V. N. Timchenko, L. V. Bystryakova.
Infectious diseases in children.
- "SpetsLit"
, 2001. - pp. 285-296. — ISBN 5-299-00096-0. - Crump JA, Luby SP, Mintz ED. The global burden of typhoid fever. Bull World Health Organ 2004; 82: 346-353.
- E. P. Shuvalova.
Infectious diseases.
- “Medicine”
, 2005. - pp. 70-88. — ISBN 522-504-00-63. - N. D. Yushchuk, Yu. Ya. Vengerov.
Infectious diseases.
- “Medicine”
, 2003. - pp. 64-73. — ISBN 5-225-04659-2. - Zh. I. Vozianova.
Infectious and parasitic diseases.
- “Health”
, 2000. - T. 1. - P. 340-379. — ISBN 5-311-011-696. - "Enterosorption" ed. prof. ON THE. Belyakova - L., 1991. - 336 p.
Dispensary observation of those who have recovered from the disease
The cessation of bacterial excretion is temporary and may resume after some time (up to several years). Convalescent drugs are prescribed against the background of complete clinical recovery, normalization of laboratory parameters, after 3-fold negative cultures of feces, urine and a single culture of bile, but not earlier than the 21st day of normal body temperature. After discharge from the hospital, those who have recovered from the disease are subject to dispensary observation; after 3 months, a bacteriological examination of feces, urine and bile is carried out. If the results are negative, observation is stopped. Convalescent workers from food and similar enterprises are under supervision throughout their entire work activity. In the 20th century, several outbreaks of disease were known to be caused by healthy carriers, some of the most famous healthy carriers being the so-called Typhoid Mary and Typhoid John.
Prevention
An effective and preventive measure against infection with typhoid fever is vaccination against salmonella. It is carried out according to epidemic indications and in areas with a high incidence rate. If necessary, the first vaccination is given to children who have reached the age of two; a second injection of the drug is indicated after a year. According to indications, adults are also vaccinated.
An important rule for the prevention of typhoid fever is following basic hygiene. This includes washing hands and food, boiling running water, adequate heat treatment of meat and fish, and observing their expiration dates.
Pathogen carrier
Recently cured patients are considered to be carriers of the bacilli. After recovery, a person remains infectious to others for a long time.
Vaccinated people are also carriers of the harmful microorganism.
In rare cases, the disease is hidden. The patient does not have severe symptoms. Treatment is carried out at home, without going to doctors and aggravating the general condition. As a result, family members and other people get sick. Most often, infection occurs through food and common household items.
Why is my child's immune system weakened?
Many people are familiar with these situations:
- As soon as the cold season begins, your child will definitely get sick
, and then the whole family. - It seems like you are buying expensive drugs, but they only work while you drink them, and after a week or two the baby gets sick again
. - You worry that your child’s immunity is weak
, very often illnesses take precedence over health. - You are afraid of every sneeze or cough.
It is necessary to strengthen YOUR CHILD'S IMMUNITY!
Salmonella typhi is characterized by a stable antigenic structure: the presence of O and H antigen. Only the causative agent of typhoid fever has a so-called virulence antigen (Vi antigen). In difficult diagnostic cases, performing serological reactions with this particular antigen makes it possible to distinguish typhoid fever itself from paratyphoid fever.
Salmonella typhi can be distinguished from other types of salmonella by certain biochemical properties. The microbiology, or more precisely the biochemistry, of the pathogen is reflected in the international Kaufman classification of Salmonella.
The causative agent of typhoid infection grows well on the most common (traditional) nutrient media, but best of all on those that contain bile. The characteristic external features of Salmonella typhi colonies have not been described.
This microbial agent is quite resistant to environmental factors. For several months it remains active in water (including well and tap water), on the surface of unwashed fruits, berries and vegetables. It dies quite quickly when treated with high temperature, various disinfectants and ultraviolet radiation.
Differential diagnosis
Typhoid fever is differentiated from a large number of diseases accompanied by prolonged fever and signs of intoxication, in particular from:
- pneumonia;
- sepsis;
- flu;
- typhus;
- brucellosis;
- leptospirosis;
- appendicitis;
- malaria;
- tuberculosis;
- infectious mononucleosis;
- lymphogranulomatosis.
To confirm the diagnosis, especially in the case of an erased or atypical course of the disease, laboratory tests are required.
Differences between typhoid fever and other diseases - table
| Typhoid fever | Flu | Pneumonia | Adenovirus infection | Tuberculosis | Malaria | |
| Seasonality | Summer–autumn. | Winter. | Cold season. | Autumn-winter. | Absent. | May - September. |
| Chills | Rarely. | Often. | Often. | Uncharacteristic. | Characteristic. | Characteristic. |
| Headache | Moderate. | Strong. | Moderate. | Weak. | Moderate. | Strong. |
| Pain | Uncharacteristic. | Expressed. | Moderate. | Possible. | Possible. | Expressed. |
| Duration of fever | 4–6 days, 5–6 weeks. | Up to 5–6 days. | 3–7 days. | 3–14 days. | Long lasting. | Up to 3–4 weeks. |
| Maximum fever (term) | Second week. | 1–2 days. | 3–5 days. | Indefined. | Indefined. | During an attack. |
| Cough | Dry, rare. | Dry, then productive | Dry, then productive | Dry, productive | Dry | Uncharacteristic |
| Dyspnea | Absent. | Possible. | Characteristic. | Absent. | Characteristic. | During an attack. |
| Skin on the face | Pale. | Blushed. | Blushed. | Not changed. | Pale. | Turns red during an attack. |
| Eye shells | Not changed. | Scleritis, conjunctivitis. | Redness. | Membranous conjunctivitis. | There are no characteristic changes. | Scleritis, conjunctivitis. |
| Lymph nodes | Not enlarged. | Not enlarged. | Not enlarged. | Enlarged. | Possible polyadenopathy (multiple damage to the glands). | Not enlarged. |
| Breath | Hard breathing, isolated dry wheezing. | Hard breathing, isolated dry wheezing. | Moist rales, breathing sounds. | Hard breathing, dry wheezing. | Hard breathing, isolated dry and wet wheezing. | The changes are not typical. |
| Heartbeat | Relative bradycardia. | Relative bradycardia. | Tachycardia. | The changes are not typical. | Tachycardia. | Tachycardia. |
| Hepatosplenomegaly (enlarged spleen and liver) | Typical. | They don't watch. | Rarely. | Often. | Possible. | Constantly. |
| Blood picture | Aneosinophilia (absence of granular leukocytes in the blood), relative lymphocytosis. | Leukopenia, lymphocytosis (increase in the number of lymphocytes in the blood). | Leukocytosis (increase in the number of leukocytes), increased ESR. | Non-specific. | Non-specific. | Anemia. |
Information sources
| : Incorrect or missing image | This article lacks links to sources of information. Information must be verifiable, otherwise it may be questioned and deleted. You may edit this article to include links to authoritative sources. This mark is set May 13, 2011 . |
K:Wikipedia:Articles without sources (type: not specified)
Symptoms and diagnostic features during pregnancy
The manifestations and diagnosis of typhoid fever in pregnant women are no different from those described above. But the disease may last a little longer than usual. However, this does not mean that it does not pose a threat to the mother and fetus.
Infection with typhoid fever significantly increases the risk of miscarriage and complications. Even if the fetus can be saved, and the most dangerous period (the second and third weeks of the disease) goes smoothly, this does not mean that the disease will not affect the health of the child and labor.
Fever, characteristic of the pathology, can provoke fetal death, especially in the early stages
Prevention of typhus
To prevent typhus, isolation and hospitalization of the infected population are used, and in parallel, a number of measures are taken against pediculosis (a lice-borne disease).
As a routine program, all children in preschool institutions and schools are subject to medical examination. If at least one case of infection is detected, the premises where the person recently stayed, his personal belongings are disinfected, and the people around him are examined.
Prevention of typhus also includes local and regional measures to identify and disinfect areas of lice accumulation. They often resort to vaccinating the population against this disease. Persons aged 16 to 60 years are routinely vaccinated against typhus.
Diagnostics
The main methods for diagnosing typhoid fever are:
- lab tests;
- bacteriological examinations of blood, feces, urine, duodenal contents;
- serological reactions.
Laboratory
Standard methods for diagnosing most diseases, including typhoid fever, are general blood and urine tests - CBC and OAM. It takes little time to take them and obtain results, so thanks to them you can get the first information about the patient’s condition within a few hours after contacting a medical facility. Subsequently, they are prescribed to monitor the dynamics of the disease at different intervals.
Typhoid fever is characterized by an increase in:
- erythrocyte sedimentation rate (ESR);
- the number of leukocytes in the first days (subsequently their level drops below normal);
- lymphocyte count;
- platelet count.
Urinalysis shows an increase in the number of proteins, casts and red blood cells.
Bacteriological
Isolation of typhoid bacilli in feces and blood is one of the main methods of confirming the diagnosis, especially against the background of a characteristic clinical picture. Therefore, blood for microbiological testing is taken immediately after the patient seeks medical help.
To isolate a blood culture, 10 ml of blood is placed on 100 ml of nutrient medium containing bile. In the laboratory, vials with cultures are placed in a thermostat, periodically reseeding. Final test results are available after 7 days, although interim data can be obtained after 3 days.
Appearance of typhoid bacillus colonies on agar
The causative agent of the disease can be detected in the blood throughout the entire febrile period. Therefore, if necessary, the study is repeated several times.
Typhoid bacilli can be isolated from feces and urine at any stage of the disease, including the first days after infection, but usually the study is carried out from the second week of the disease, and then repeated many times until discharge from the hospital. To do this, the samples taken are sown on solid nutrient media, as a result of which colonies of pathogens grow on them.
Preliminary results of bacteriological studies can be obtained 2 days after taking the material, final results - after 4 days.
Serological
This type of diagnosis is informative already from the end of the first week of the disease. Its essence is to carry out the so-called Widal reaction - a method for detecting antibodies (agglutinins). The starting material for them is venous blood. But since, due to the individual characteristics of patients, the increase in antibody concentration to minimum diagnostic values may be delayed, serological diagnostic methods are used only as an aid in identifying typhoid fever. Serological tests are repeated at 3–4 weeks. They are used to evaluate the dynamics of the disease. Test results are usually ready in 18–20 hours.
From the first days, it is possible to detect pathogens in biological fluids by performing immunofluorescence microscopy and enzyme-linked immunosorbent assay (ELISA). They are based on the identification of specific antigens in biological samples, and they are highly sensitive, thanks to which these tests can be used for rapid diagnosis during epidemics.
Types of typhus
Scientists divide the disease into 2 types:
- Endemic typhus (rat);
- Epidemic typhus.
The causative agents of the first type of disease are rickettsia R. Mooseri. In the United States, about 40 people become sick with typhus every year. The largest number of patients was recorded in regions with a warm climate, especially in the warm season and in rural areas. The symptoms and course of the disease are much milder than in the case of epidemic typhus. A person becomes infected when bitten by rat fleas, the carriers of the virus.
Epidemic typhus is also known as European, classical or louse fever, and as prison or ship fever. The causative agent of the disease is Rickettsia prowazekii.