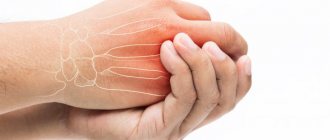
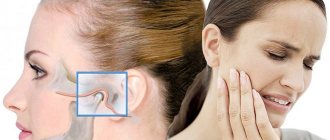
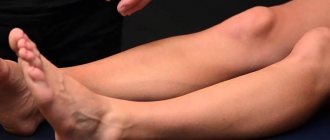
The main task of a dental surgeon during the treatment of a fracture of the upper or lower jaw is to restore the anatomical structure of the broken bone and the correct relationship of the dentition. Many techniques help to achieve this, but the effectiveness of treatment also depends on how correctly and quickly first aid was provided.
Before hospitalization
First aid to the victim includes:
- stopping bleeding (pressing or packing the wound, applying cold);
- if necessary, cardiopulmonary resuscitation;
- pain relief (analgin, revalgin intramuscularly);
- immobilization of the jaw with the help of fixing bandages (contraindicated if the victim is unconscious, since this increases the risk of suffocation from the retraction of the tongue or vomit entering the respiratory tract).
First aid
The likelihood of complications and how long treatment and recovery will take depends on how timely and correctly the first aid is provided to the victim. Emergency assistance consists of:
- Disinfecting the wound and applying a bandage to it to prevent infection.
- Pain relief. To relieve pain, you can use non-steroidal anti-inflammatory drugs such as Ketorolac, Diclofenac. To enhance the analgesic effect, injections are recommended. In cases where a fracture is associated with serious complications, it is necessary to use potent drugs, for example Promedol.
- Stop bleeding. In order to stop the bleeding, you should press the bleeding vessels with your finger and apply a pressure bandage. If the bleeding is not strong, you can limit yourself to a piece of sterile cotton wool soaked in hydrogen peroxide.
- After the bleeding stops, the broken jaw must be fixed. For this purpose, it is better to use a sling-shaped bandage.
The jaw is fixed with a sling-shaped bandage (as tightly as possible);
- Bleeding (if any) is stopped - sterile bandages and tampons are used. If the bleeding is severe, you need to press the adductor artery (with your finger);
- The oral cavity must be cleared of tooth fragments, blood clots, and vomit;
- If the victim is unconscious and the tongue sinks, turn the patient on his side so that he does not suffocate.
- It is advisable to apply ice or a cold compress to the affected area.
By this time, the ambulance should have arrived. In such cases, they are taken to maxillofacial surgery.
Surgeons combine the bone fragments, then rigidly fix the fragments in one way or another. The patient is prescribed antibiotics to prevent soft tissue infection, as well as rest to ensure normal recovery of the body.
Emergency measures for the injured include preventing shock, as well as possible and associated suffocation. In case of loss of consciousness, it is necessary to ensure that the patient’s sunken tongue does not block the airway. To avoid suffocation in an unconscious state, he is placed on his side and his tongue is fastened.
If a patient has significant blood loss, it is necessary to locate the lesion and clamp the nearby artery or cover the bleeding wound with cotton wool or a bandage.
Having eliminated all kinds of life-threatening symptoms, it is necessary to immobilize the injured jaw. To do this, use special bandages or improvised means (handkerchief, bandage, scarf) that can reliably immobilize the organ.
It is advisable to apply ice or a cold compress to the injury site. Having provided first aid to the patient and made sure that his life is not in danger, you can wait for the doctors to arrive or on your own, send the patient to a medical facility.
At the first sign of a fracture, contact a specialist immediately. If bleeding is observed, it must be eliminated as soon as possible.
What to do?
Hold your jaw with your hand or a homemade bandage and wrap it around the injured area until medical professionals arrive. Do not attempt to talk, eat, or move your jaw to avoid complicating the injury by causing tooth decay and additional displacement. If possible, take painkillers.
Osteosynthesis
Indispensable for complex, comminuted and multiple fractures with displacement, loose teeth and complete absence of teeth, for periodontal disease and other inflammatory diseases of the gums in the area of injury. Osteosynthesis is also effective in cases of fracture of the condylar process complicated by dislocation of the articular head of the lower jaw.
Fastening materials can be steel knitting needles and rods, pins, nitride-tinan wire with shape memory, quick-hardening plastics, polyamide thread, special glue.
However, osteosynthesis with metal miniplates is considered the most convenient and safe method today. They allow you to cut through the skin and muscles on only one side, which simplifies the operation itself and shortens the recovery period. Another undeniable advantage is the ability to reliably fix fragments in areas with significant dynamic loads.
Nosebleeds
Nosebleeds
– the most common types of bleeding encountered in the practice of any doctor.
Depending on the reasons that caused the bleeding, a distinction is made between traumatic
(mainly local) and
symptomatic
(both general and local) nosebleeds.
Traumatic nosebleeds
occur as a consequence of any injury.
This includes injuries to the nose of a domestic, industrial, transport nature, or during surgical interventions in the nasal cavity. Bleeding can occur when removing crusts from the anteroinferior sections of the nasal septum with a finger; perforations often occur here against the background of atrophic processes or after septoplasty, which can also be a source of bleeding. Symptomatic bleeding
is usually a manifestation of some physical disease.
Most often these are cardiovascular diseases (arterial hypertension, atherosclerosis), kidney diseases (nephrosclerosis, renal hypertension), diseases of the blood system and changes in the vascular wall (hemophilia, Osler-Rendu disease, hemorrhagic thrombosthenia, Werlhof's disease, hemorrhagic vasculitis, Schonlein disease – Henoch, capillary toxicosis, hemorrhagic telangiectasia), diseases of the hematopoietic organs (leukemia, reticulosis, hemacytoblastosis, etc.). To establish a diagnosis for prolonged bleeding of unknown etiology, additional studies are carried out, such as a biopsy from the area of bleeding, a coagulogram, a thromboellastogram, etc. Nosebleeds can be an early sign of a nasal tumor. The most dangerous are post-traumatic nosebleeds when an aneurysm of the afferent vessels of the nose has formed (aneurysm of the cranial branch of the branches of the internal carotid artery, cavernous-carotid aneurysm). These bleedings are especially profuse and persistently recur. A sign of nosebleeds is the flow of scarlet, non-foaming blood from the vestibule of the nose or the flow of blood down the back wall of the pharynx when the head is thrown back. With prolonged, especially hidden nosebleeds, even not very heavy ones, a collaptoid state develops: pale skin, cold sweat, weak rapid pulse, drop in blood pressure. Usually, with anterior rhinoscopy, it is possible to identify the site of bleeding if it is located in the anterior third of the nasal septum. If the source of bleeding is located in the deep parts of the nasal cavity, then it is more difficult to determine. Depending on the volume of blood loss, there are: • minor bleeding
, which occurs more often from the Kisselbach area;
blood in a volume of several milliliters is released in drops for a short time; Such bleeding often stops on its own or after pressing the wing of the nose to the septum; • moderate nosebleeds
are characterized by more abundant blood loss, from several tens of milliliters to 200 ml in an adult, while hemodynamic changes are usually within the physiological norm;
Splinting the jaw
This is the immobilization (fixation) of bone fragments using a special plastic or wire structure.
The technique, created by military doctors at the beginning of the 20th century, is successfully used by dentists today. The materials used to make the splint have changed, and the methods of applying it have been improved.
Today, a specialist has many types of tires in his arsenal:
- from standard Vasiliev tape splints, the simplest and cheapest method of treatment;
- to aluminum Tigerschdedt splints, which are made individually for each patient, due to which they are more effective. In addition, they evenly distribute the load and minimally injure the teeth.
The type of splinting depends on the type of injury and can be unilateral (when one jaw is fractured) or bilateral (when both are damaged).
If the teeth are preserved, it is not difficult to apply a bent dental wire splint. It is bent to the shape of the dental arch and fixed with bronze-aluminum wire ligatures, which, like a hairpin, cover the tooth on both sides. Manipulations are performed under local anesthesia.
When both jaws are fractured, a structure with a more rigid base is installed; in addition to wire, hooks and rings are also used that immobilize the lower jaw.
Characteristic symptoms
Despite the fact that different types of mandibular fractures have their own characteristics, they all have a list of common features.
Among them: sudden acute pain, nausea, disturbances in chewing, swallowing, and speech functions. In a photo or with the naked eye, the incorrect position of the dentition is often visible.
The victim is unable to close his mouth. Other symptoms depend on the location of the fracture and its nature.
In particular, damage to the lower jaw has the following signs:
- swelling of soft tissues,
- symmetry violations,
- bleeding,
- pain when pressing, talking and opening the mouth,
- malocclusion,
- tooth sensitivity,
- increased salivation with blood.
How to treat a broken nose is described in detail here
If the upper part of the jaw is broken, the symptoms will be as follows:
- bleeding in the area between the upper lip and teeth,
- swelling of the nose, cheeks, lips,
- possible displacement of the nasal septum, fracture of the maxillary sinus,
- hematoma under the eyes (in case of touching the base of the skull),
- impairment of smell, vision,
- loss of ability to open mouth,
- drooping eyeballs,
- asymmetrical face.
Is it possible to do without splinting?
Even if the case is not severe - the fracture is one-sided, closed and without displacement - it is imperative to take measures to prevent the development of such unpleasant complications as:
- accidental displacement of fragments,
- re-injury
- development of inflammation of soft tissues,
- infection of the fracture site.
To do this, it is necessary to immobilize the jaw by any available method. This can be a sling bandage, but it is much more convenient and effective to use a splint. In case of a complicated fracture, splinting is absolutely indispensable, regardless of the location of the injury.
Possible complications
Complications can often occur after a bone injury. The most common are:
- external bleeding,
- hematomas at the site of injury,
- dislocations of the temporomandibular joint,
- osteomyelitis, which occurs due to infection.
- the appearance of a malocclusion,
- pseudarthrosis,
- displacement of the dentition,
- improper bone fusion
- neuritis of the nerve, which can cause loss of sensation,
Treatment tactics for displaced fractures
In such cases, before applying a splint, it is necessary to compare the jaw fragments, for which reduction orthopedic devices are used. A broken upper jaw requires traction using special dental splints.
Such injuries are very dangerous because they can cause asphyxia. But correctly provided first aid will prevent suffocation. Clear the oral cavity of foreign bodies or blood, lay the victim face down, placing a cushion rolled up from clothes, blankets, etc. up to the chest.
Types of fractures
The classification of fractures of the upper jaw makes it possible to determine the characteristics of the damage, as well as some nuances in the treatment of such a condition. At the moment, there are three types of damage. Among them:
- Le Fort 1 – an upper fracture of the bones of the upper jaw is performed. Usually occurs due to damage to a portion of the orbit or due to an oblique blow to the face. The maxillary-zygomatic complex moves away from the skull, and the patient exhibits signs of neurological abnormality.
- Le Fort 2 – medium fracture of the upper jaw. It occurs against the background of a direct blow to the nasal bones when the mouth is closed. In addition, such a fracture is diagnosed with a reflected lesion of the chin. This type of jaw fracture is characterized by separation of the mass.
- Le Fort 3 – lower fracture of the upper jaw. Usually occurs when there is a strong blow to the open jaw.
Rehabilitation after a jaw fracture
For successful treatment of a jaw fracture, anti-inflammatory and restorative therapy, physiotherapy, mechanotherapy and special oral hygiene are also important.
- Within 3-4 days after the injury, antibiotics must be prescribed to prevent inflammation, which are injected directly into the area of injury.
- General strengthening therapy is taking vitamins C, P, D and group B, drugs that stimulate tissue regeneration and restore the level of leukocytes in the blood.
- Among the effective physical procedures, we note UHF therapy, general ultraviolet irradiation, and magnetic therapy. After the third procedure, swelling and pain are noticeably reduced, swelling subsides. For better healing of fragments, 2 weeks after a jaw fracture, electrophoresis is performed using a two to five percent solution of calcium chloride.
- Mechanotherapy, or physical therapy, accelerates the restoration of jaw function and helps if, after an injury, the mouth opens poorly or does not open at all. It can also be practiced at home, starting 4-5 weeks after the fracture, when the splints are removed and a callus has formed.
- Special hygiene involves irrigation at least 8-10 times a day. For unconscious victims, their teeth and mucous membranes are treated with a special solution at least twice a day.
Diagnosis of injury
A jaw fracture is one of those injuries, the presence of which can be determined without the presence of special instruments. But in order to carry out high-quality treatment and accurately determine the degree of complexity of the injuries and their features, you need to undergo a thorough examination by a doctor. After a visual inspection, he will prescribe the most effective method for identifying cracks. For example:
- x-ray,
- orthopantomography,
- CT,
- MRI.
It is clear that if the fracture is caused not by external factors, but by internal failures, then the doctor will additionally prescribe other tests. This is the only way to identify the real cause of the injury.
In addition, if the symptoms have reached other organs, then it is also worth going to a neurologist, otolaryngologist and ophthalmologist. During the examination, the blood pressure level is also monitored.
How to eat?
Since during intensive therapy and during the recovery period the jaws are rigidly fixed and habitual chewing of food is out of the question, correction of the diet is necessary during this period.
Food should have the consistency of low-fat sour cream. These are broths, pureed soups, carefully chopped vegetables and fruits, milk drinks, liquid cereals. Spices are excluded, salt consumption is limited. The temperature of the dish should not be higher than 45-50 °C. The most convenient way to eat food is through a straw.
You need to gradually switch to your usual diet after removing the splint. This is important not only for restoring chewing functions, but also for preventing disorders in the gastrointestinal tract.
Oral care for a fracture
Oral hygiene plays an important role during rehabilitation. Leftover food serves as a breeding ground for pathogenic microflora. This can cause an inflammatory reaction with the formation of ulcers. An additional aggravating factor is metal structures (knitting needles, wire), which fix the bones and can cause bedsores on the gums.
Treatment of the oral cavity is carried out by medical personnel (during dressings) and by the patient himself. The following antiseptic solutions are used: 3% hydrogen peroxide solution, potassium permanganate solution, furacillin, chlorhexidine, etc.
Treatment must be performed with a syringe or rubber bulb. It is not recommended to use gauze or cotton balls, as their fibers will remain on metal structures.
It is important that the patient rinses his mouth not only after each meal, but also in between meals. Remains of food stuck between the teeth should be carefully removed with a toothpick.
In addition, it is necessary to regularly brush your teeth with hygienic paste and a toothbrush. The absence of bad breath indicates that the oral cavity is being treated correctly.
How much does it cost to treat a broken jaw?
The price depends on the nature of the injury, whether osteosynthesis was performed, what splints were used, and whether the patient attended physical therapy procedures. But let's say for sure that the service is not cheap. Osteosynthesis alone will cost from 14,000 to 55,000 rubles.
It is also necessary to consider the cost of subsequent dental treatment to restore lost teeth or damaged teeth after splinting. Our service will help you choose a competent specialist and not waste your money. Compare prices and services of different clinics, read reviews from real patients.
Anatomical features of the structure of the upper jaw
To understand the specifics of the injury, you need to know the structural features of the upper jaw. So, the upper jaw is a paired bone that has connections with several bones of the facial skull: the sphenoid, ethmoid, zygomatic, frontal and nasal. At the places where they connect, so-called bone sutures are formed.
It is in the places of bone sutures that the fracture lines pass. This is explained by the fact that these areas have less strength and are easily injured by mechanical stress.
In addition, the presence of bone sutures on the facial skull determines the combined nature of the injury. An isolated fracture of the upper jaw is rare; more often it spreads to adjacent bones.
The second anatomical feature of the upper jaw is the abundance of blood vessels. As a result, fractures are accompanied by intense bleeding . Moreover, trauma is characterized by both external and internal bleeding. The latter have an unfavorable prognosis: firstly, such bleeding cannot always be detected in a timely manner, and secondly, technical difficulties often arise when stopping it.
Signs according to the Le Fort classifier
- sensation of a foreign body in the throat;
- blood mesh around the eyes;
- impaired vision, double objects;
- swelling of the entire face;
- lack of swallowing reflex, pain when opening the mouth;
- eyeballs are displaced;
- modification of the contour, lowering of the jaw, lengthening of the face;
- when palpating the facial bones, movement and a specific sound (crunching) in the area of the nose and eye sockets are noticeable.
- lack of sensitivity of the nose and lips;
- failure to recognize odors;
- hematomas on the lower eyelids;
- bleeding from the nose and mouth;
- crunching (crepitus) in the area of the nasofrontal suture.
- swelling of the face and lips;
- absence of nasolabial fold;
- acute pain;
- change in bite;
- pain when moving the jaw;
- difficulty opening the mouth.
When diagnosing various fractures, as a rule, an X-ray image is sufficient. With a jaw injury, everything is much more complicated. Conventional radiography is problematic due to the structure of the facial skeleton and the layering of one bone on top of another. Here they use an overview projection showing the front of the skull. But a plain radiograph is not enough, because it cannot identify fragments that have fallen inside the skull.
MRI and computed tomography assist in diagnosis. Their resolution makes it possible to simultaneously detect damage to both the facial and intracranial bones.
Read also: How babies lose teeth
Osteoma of the condylar process of the mandible
Osteoma is a benign tumor of bone tissue, occurring in 2.7-5.9% of patients with benign tumors of the facial bones. Currently, it is suggested that the number of true osteomas is significantly smaller, since this diagnosis is often mistakenly made in cases of reactive hyperplasia, exostoses of the jaws, and some forms of fibrous dysplasia [3, 17].
Osteomas, as a rule, grow very slowly and painlessly, without making themselves felt for a long time. Their clinical picture is mild and depends on the location and size of the tumor. Developing in the area of the body of the lower jaw, osteomas lead to deformation of the corresponding area, aesthetic and functional disorders. Osteomas of the upper jaw with significant sizes cause exophthalmos, diplopia, lacrimation, impaired nasal breathing and neuralgic pain due to compression of the branches of the trigeminal nerve. When localized in the area of the frontal sinus and ethmoid labyrinth, the tumor is capable of deforming the walls of the sinuses, destroying them, growing into the orbit and cranial cavity [3, 15].
Damage to the condylar process of the mandible is quite rare and is characterized by specific symptoms. Osteomas of this localization present a certain difficulty for diagnosis and surgical treatment, remaining asymptomatic for a long time, but in later stages they can cause severe aesthetic and functional disorders [3, 9, 17].
Osteoma of the condylar process was first described in detail by Eckert (1899), pointing out displacement of the lower jaw, impaired mouth opening, as well as changes in facial contours on the side of the lesion of the condylar process of the mandible among its main clinical manifestations [1]. Subsequently, a few reports were presented in the literature, mainly about isolated observations of this disease [1, 11, 13, 14]. Deboise A. (1981), noting that osteoma is the most common benign neoplasm of the structures of the temporomandibular joint (TMJ), provides only 3 of his own observations [9]. The largest number of clinical observations of osteomas of the condylar process - 23 - belongs to H. Zhang (1997) [18]. The author, however, does not indicate whether in all cases the diagnosis of true osteoma was confirmed histologically.
Clinical observation
Patient K., 36 years old, medical history No. 4408 dated March 19, 2004, was admitted to the maxillofacial department No. 2 of City Clinical Hospital No. 12 in Kiev with complaints of facial deformation due to displacement of the lower jaw, malocclusion, difficulty chewing food, crunching in the left TMJ, moderate pain with increased load on the joint. For the first time, he noticed a facial deformity—a displacement of the chin to the right—in November 2002. Later, a clearer clinical picture emerged; the severity of the displacement and malocclusion slowly progressed until the moment of treatment. Objectively, the patient had pronounced facial asymmetry due to displacement of the lower jaw to the right (Fig. 1).
Rice. 1. The chin is shifted to the right side, a state of physiological rest.
In the pretragus area, the laterally displaced head of the left TMJ was clearly palpated. Mouth opening was up to 4.5 cm, with a crunch in the area of the left TMJ and a Z-shaped deviation of the lower jaw. Lateral movements of the jaw to the right were limited, the bite was oblique, and the midline shifted to the right by 1 cm (Fig. 2).
Rice. 2. In the pretragus area, the laterally displaced head of the left TMJ is clearly palpated.
A series of radiographs (orthopantomogram, radiograph of the mandible in direct projection and in the Haenisch position on the left, computed tomogram of the joint area with 3D reproduction) revealed a shadow of bone density with a size of 2x1.7 cm, associated with the left condylar process and located in the infratemporal fossa. The structures of the left TMJ were preserved, although somewhat deformed. When planning surgical intervention, a stereolithographic model of the patient’s skull was made (Fig. 3), on which the necessary measurements were made and the surgical approach was determined.
Rice. 3. Stereolithographic model of the skull, neoplasm of the left condylar process of the mandible.
On March 23, 2004, the patient underwent surgery: removal of a neoplasm of the condylar process of the lower jaw under endotracheal anesthesia with intubation through the nose. To do this, a preauricular and semicoronal approach was provided to the zygomatic arch, which was then resected and displaced downward on the fibers of the masseter muscle (Fig. 4).
Rice. 4. Surgical wound, coronal access, osteotomy of the zygomatic arch: 1 - zygomatic arch, 2 - osteotomy areas.
The fibers of the temporalis muscle were partially transected and detached, allowing access to the infratemporal fossa, where a bone formation was visualized anterior and medial to the head of the jaw (Fig. 5).
Rice. 5. The area of the infratemporal fossa, access to the tumor has been created.
The tumor is separated from the soft tissues and fixed using a special bone fixation made in the form of a corkscrew (Fig. 6).
Rice. 6. Macroscopic specimen of osteoma of the condylar process of the mandible.
The tumor was removed within the healthy bone. The zygomatic arch is placed in place and fixed with two wire bone sutures. The soft tissue flap was put in place, the wound was sutured in layers. The postoperative period proceeded without complications. Closing of the jaws in the correct position was noted the next day after surgery without any orthopedic measures (Fig. 7).
Rice. 7. State of physiological rest of the lower jaw on the first day after surgery. Closing of teeth in a physiological occlusion with restoration of the midline.
The radicality of tumor removal was confirmed by computed tomography data (Fig. 8).
Fig.8. Facial symmetry, state of physiological rest, 9 years after surgery.
Vertical movements of the lower jaw were fully restored on the 5th day. There was a slight paresis of the frontal and zygomatic branches of the facial nerve, the function of which was completely restored on the 7th day after surgery. Postoperative swelling of the temporal and zygomatic areas persisted for 8 days. On April 2, 2004, the patient was discharged in satisfactory condition with recommendations for rational prosthetics.
On January 16, 2013, patient K. underwent a repeated scheduled examination using clinical and instrumental research methods. The patient did not have any complaints from the TMJ. On bilateral palpation of the TMJ, no crunching or crepitus was observed, and there were no pain symptoms. Objectively: the contours of the face are symmetrical, the maximum opening of the mouth is 4 cm (Fig. 9, 10), the midline of the face is restored, the movements of the lower jaw are not limited, without signs of lateral deviation.
Rice. 9. Maximum mouth opening, 9 years after surgery. Rice. 10. Orthopantomogram, 9 years after surgery.
According to an orthopantomogram and computed tomography in 3D reconstruction mode, the structural elements of the left TMJ have clear anatomical contours and the structure of bone tissue is within normal limits. The relationship between the condylar process and the glenoid fossa ensured the functional stability of the TMJ and was considered acceptable (Fig. 11, 12).
Fig. 11. Computed tomography data. Rice. 12. 3D reconstruction of the skull, 9 years after surgery.
Discussion
Localization of osteoma in the TMJ region is a rare clinical situation. The paucity of clinical symptoms characteristic of osteomas determines the dominance in the clinical picture of nonspecific functional disorders of the TMJ, which makes it necessary to carry out differential diagnosis with other diseases of the joint - hyperplasia of the branch, deforming arthrosis, ankylosis, intra-articular disorders, habitual dislocation, etc. X-ray studies in standard settings are quite informative for making a correct diagnosis, but are clearly insufficient for choosing a method of surgical treatment. To clarify the localization of the tumor, taking into account the changed anatomical relationships, its relationship with the elements of the joint and the nature of structural changes in the latter, it is necessary to conduct computed tomography with 3D reconstruction. A thorough examination allows you to decide on further surgical tactics.
When the osteoma is anteromedial in relation to the condylar process, it is located in the region of the infratemporal fossa. Removing the tumor in this case is associated with significant difficulties, and sometimes even with a risk to the patient’s life. Chen Y. (2003) states that when the tumor is localized in the area of the articular process, in most cases its resection followed by arthroplasty and orthopedic treatment is indicated [8]. Other authors adhere to the same point of view, recommending combining resection of the condylar process with subsequent plastic surgery of the joint, lengthening of the ramus, combined operations on the upper and lower jaw to correct the bite and hardware treatment [4, 7, 18]. At the same time, the above observation indicates that in some cases it is possible and even necessary to remove the tumor while preserving the elements of the joint. This is also evidenced by the data of Piattelli A. (1995) and other authors [11, 13].
It should be noted, however, that when the osteoma is anteromedial in relation to the condylar process (according to the literature, this is the most typical localization), it is located in the region of the infratemporal fossa. This area is surgically extremely difficult to access and is located near vital structures, so removing the tumor in this case is associated with significant difficulties and sometimes even a risk to the patient’s life.
The main anatomical obstacles to reaching the infratemporal fossa are the zygomatic arch, the ramus of the mandible, the parotid gland and the facial nerve - formations that are extremely important in functional and aesthetic terms. Access to the tumor should be sufficient for its radical removal and provide a good overview.
Currently, a number of options for surgical access to the infratemporal fossa have been proposed, more or less satisfying these requirements, but not all of them are appropriate in the case of osteoma of the condylar process.
In 1961, JF Barbosa developed an approach to the infratemporal fossa, which involved performing a Weber-Fergusson incision followed by mobilization of the zygomatic complex and resection of the mandibular ramus [6]. DJ Crockett (1963), using a similar approach, limited the resection of the branch to the coronoid process only [10, 16]. This so-called anterior route is usually combined with maxillary resection and provides a wide view, but at the same time it is very traumatic and unfavorable from a cosmetic point of view. The infratemporal fossa can also be achieved by making a premaxillary incision followed by osteotomies of the mandibular ramus at various levels, rotation or removal of the bone fragment from the surgical site. In case of resection of a section of the branch, the latter can be returned to its place at the end of the operation and fixed in the form of a free autograft [16].
The main anatomical obstacles to reaching the infratemporal fossa are the zygomatic arch, the ramus of the mandible, the parotid gland and the facial nerve - formations that are extremely important in functional and aesthetic terms. In 1985, NR Attenborough proposed the use of a coronal approach to visualize the structures of the pterygopalatine and infratemporal fossa. This method involved making pre-auricular and semi-coronal incisions with subsequent removal of the zygomatic arch and coronoid process [5]. HL Obwegeser improved this technique by combining mobilization of the entire zygomatic complex with osteotomy of the coronoid process. In this case, the zygomatic bone was displaced downward on the fibers of the masticatory muscle, and the coronoid process was retracted upward [12]. In addition to the above, numerous modifications and combinations of access are used depending on the clinical situation [10]. As our experience shows, the use of coronary access is the method of choice when removing tumors localized in the infratemporal fossa. It provides a good overview and freedom of surgical manipulations, avoids injury to large vessels and branches of the facial nerve, and is also most cosmetically acceptable.
We also note that with long-growing bone tumors in the TMJ area, the joint can undergo significant morphofunctional changes that require postoperative orthopedic correction, however, as was shown in our observation, the compensatory capabilities of the joint are quite high, which in some cases with low-traumatic and radical removal tumor allows you to achieve restoration of function without additional measures in the postoperative period.
Thus, observation of the patient in the long term after surgery (9 years), indicating a relapse-free course and the absence of deep functional disorders, confirms the effectiveness of the approaches used to remove the TMJ tumor. Careful diagnosis and surgical intervention using approaches that provide wide access to the infratemporal fossa allowed for radical removal of osteoma of the condylar process of the mandible, while avoiding additional trauma to the anatomical formations of this localization, providing a quick postoperative recovery period and a satisfactory result for 9 years with complete restoration of TMJ function.
Materials used
Currently, there is a large selection of materials that can be used for splinting. Each experienced doctor has his own set of favorite materials with which he is accustomed to working and achieves a certain result.
Splinting with fiberglass
But we must understand that materials are selected depending on the degree of injury, as well as the individual characteristics of the patient. What helps one patient will not always save another. Therefore, the selection of special materials is carried out by the attending physician.
The list of popular materials for splinting includes metal wires, plastic parts, fiberglass tapes, rubber bands for fixation, and metal hooks or rings.
Causes
A fracture of the jaw bones can be caused by a huge number of reasons. Doctors divide such damage into traumatic and pathological. Violation of the integrity of the jaw bones without injury can be caused by the following:
- Benign and oncological neoplasms;
- Genetic abnormalities;
- Tuberculosis and osteomyelitis;
- Cysts;
- Insufficient nutrition, deficiency of necessary elements;
- Metabolic disease;
- Infectious infections;
- Therapy with certain medications.
In addition to harmless reasons, a jaw fracture can occur due to serious facial trauma.
Most often this happens after strong impacts, injuries, or intense stress. Traumatic fracture most often occurs in people who are actively involved in sports, drive a car, have experienced an abnormal tooth extraction, or have received a gunshot wound.
Peculiarities
No one is immune from such a fracture, but it is most common in men aged 20 to 45 years.
Reasons that lead to these injuries:
- structural features of the bone (movable arch fixed at the extreme points);
- protruding chin (it bears the brunt of the impact);
- falls, blows.
A jaw fracture is a rather dangerous injury, since if bones and their fragments are displaced, the airways can be blocked, blood vessels, nerves of the head, neck, and even the brain stem can be damaged. During a fracture, infectious complications from diseased teeth are possible, which lead to osteomyelitis (bone damage).
Violation of the integrity of the jaw bones can lead to death. This danger arises with complex fractures, which lead to other serious disorders and are accompanied by associated injuries.
A broken jaw in itself is a dangerous, but not fatal injury.
The lower jaw has certain places that are susceptible to fractures due to certain injuries. Fractures happen:
- open;
- closed;
- with offset;
- without displacement of fragments;
- splintered.
Violation of the integrity of the jaw bone and all the above-described manipulations aimed at its restoration entail great difficulties in the implementation of natural processes. Nutrition during this period should be liquid, but at the same time contain all the substances necessary for a person. You can only eat food that has been ground and diluted to a liquid state. Nutrition is provided by the following methods:
- a sippy cup with a rubber tube that is inserted directly into the stomach. It can also be used at home to feed the victim;
- gastric tube, it is installed in the hospital;
- drip, used when the patient is unconscious;
- nutritional enemas, in severe cases, when the unconscious patient does not have veins for the administration of maintenance drugs.
Nutrition also involves the presence of certain foods in the diet. During this period, food prepared at home should completely replenish the body’s daily need for microelements, proteins, and fats. This should be a complete meal containing high-calorie dishes. It is useful for the patient to eat boiled meat, dairy products, vegetables and fruits for recovery.
The task of a dental surgeon in the event of a patient’s jaw fracture is to restore the integrity of the broken bone along with the dentition.
Up to 70% of damage occurs in the lower jaw due to:
- accidents, accidents;
- blows during a fight;
- sports injuries;
- complications of serious diseases.
The collective concept of trauma combines a wide range of injuries.
Healing will be faster and more effective if symptoms are correctly recognized and time is not wasted in providing medical care.
The healing time of the jaws will differ significantly in the case of:
- direct or indirect fractures, i.e., distant from the point of impact;
- closed or open injuries, i.e. with rupture of soft tissues;
- with displacement of bone fragments or without displacement, while maintaining the anatomical location;
- a complete fracture with the advancement of a fragment with an angle, or a comminuted one (one of the most dangerous) with dispersed fragments in disarray.
An accurate assessment of the damage can be made based on the x-ray and clinical picture.
Healing times largely depend on the type of fracture and the provision of timely assistance. Soft tissue injuries, bone displacement, concussion, contusions and associated injuries increase the period of inpatient observation.
Features of jaw treatment may be associated with general diseases of the patient.
Consequences
If you have been diagnosed with a jaw fracture, you must follow all the recommendations of your doctor. Otherwise, you risk facing serious complications in the future. Most often, patients who did not adhere to the specialist’s recommendations encounter the following problems:
- Changing the location of the dentition, its displacement;
- The appearance of gaps between teeth at the fracture site;
- Malocclusion;
- Severe painful sensations in the oral cavity, which significantly intensify while talking or chewing;
- General malaise, frequent headaches, dizziness and nausea;
- Recession of the tongue;
- Loss of sensation in the lower part of the face;
- Displacement of all teeth from their usual places;
- Violation of the functions of swallowing, chewing, breathing;
- Displacement of part of the jaw.
Lack of timely treatment for a jaw fracture can provoke serious deviations in the functioning of the entire body.
First of all, patients experience a concussion, which leads to bleeding from the ears and loss of consciousness. The greatest danger is posed by complications such as osteomyelitis, meningitis and other inflammatory processes. It is for this reason that a patient with a jaw fracture should regularly visit a doctor for extensive diagnostics.
This is the only way to reduce the likelihood of complications.
Diagnostics
Diagnosis of perforation of the floor of the maxillary sinus during tooth extraction is based on a typical clinical picture. In doubtful cases, as well as when such a complication is suspected during implantation or endodontic manipulations, it is necessary to use instrumental diagnostic methods:
- Probing the socket of an extracted tooth or perforated canal with a thin probe. This allows us to determine that there is no bone bottom in the wound. In this case, the instrument passes freely through soft tissues and does not encounter obstacles along its path.
- X-ray of the sinus area. In this case, the pictures can reveal both darkening of the cavity due to the accumulation of blood in it, as well as fragments of dental roots, implants or filling material. Sometimes it is advisable to conduct radiography with contrast, when a contrast agent is introduced into the cavity through a perforation fistula.
- Computed tomography, which allows you to determine perforations and the presence of foreign bodies in the sinus with maximum accuracy.
- If old perforations are suspected, general clinical blood tests are performed, the results of which may indicate the presence of an active source of infection in the body.
Causes of perforations of the maxillary sinus floor
The etiology of perforations of the maxillary sinus is always associated with any dental procedures. Perforation can occur:
- when removing teeth;
- during endodontic treatment;
- during dental implantation;
- during root resection.
When teeth are removed, damage to the bottom of the maxillary sinus can be a consequence of either rough actions by the dentist or failure to comply with treatment tactics, or as a result of the anatomical characteristics of the patient himself (for example, when the tooth roots are located directly in the sinus cavity).
In the photo: the tooth root is located close to the bottom of the maxillary sinus, which increases the likelihood of perforation during removal
When endodontic treatment is carried out, one of the complications is perforation of the tooth root, which is often combined with damage and perforation of the bottom of the maxillary sinus. This happens when the root canals are excessively expanded, when brute force is used when inserting pin elements or compacting filling cement. With this type of perforation of the maxillary sinus, filling material or root fragments almost always penetrate into its cavity.
If perforation occurs at the time of insertion of a dental implant (it can be an implant of any brand, for example, Mis, Nobel, Xive, etc.) or during root canal filling or insertion of pins into the tooth root, then it is always a therapeutic error doctor's tactics.
Damage to the bottom of the maxillary sinus is a serious complication when implanting artificial roots into bone tissue during prosthetics. This is explained by the fact that after tooth extraction, bone tissue very quickly undergoes degeneration processes. As a result, the height of the alveolar process of the jaw decreases. If the doctor does not take this point into account and incorrectly carries out preparations before implantation, and also incorrectly selects the size of the implant, then the risk of sinus perforation is very high.
Tooth root resection is a treatment method for the presence of cysts in the area of its apex. If the patient is underexamined, when the doctor does not know the exact size of the bone plate separating the bottom of the sinus from the wall of the cyst, and also if it is necessary to remove a large volume of jaw bone, then perforation of the maxillary sinus is not a rare phenomenon.